What is Impetigo? Causes, Symptoms and Treatment
SkinChange.AI
Medical editorial team
Impetigo is one of the most common bacterial skin infections in children, but it can affect all age groups. Despite its prevalence, impetigo can be uncomfortable and — in rare cases — lead to complications if not treated properly.
In this article we explain exactly what impetigo is, what it looks like, who gets it, and what you can do about it.
What is impetigo?
Impetigo is a superficial bacterial skin infection affecting the epidermis — the outermost layer of the skin. The infection is primarily caused by Staphylococcus aureus (staphylococci) and Streptococcus pyogenes (streptococci), which enter the skin through small cracks, splinters or insect bites.
Impetigo is contagious and can spread from person to person through direct contact or via contaminated objects. The disease is, however, mild in most cases and can be treated effectively with antibiotics.
The two types of impetigo
There are two main types of impetigo:
Non-bullous impetigo (the most common)
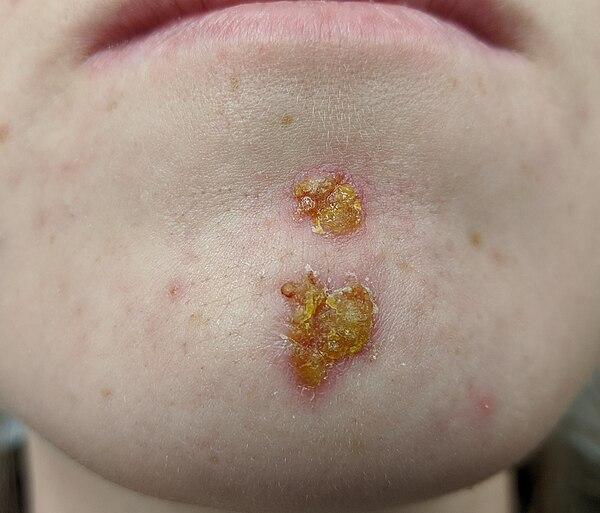
This is the most common form, accounting for about 70% of all impetigo cases. It typically starts as small red spots around the mouth and nose, which quickly develop into small blisters. When the blisters burst, they leave the characteristic honey-coloured or yellow crusts — which can resemble dried honey or wax.
Bullous impetigo
Bullous impetigo is specifically caused by Staphylococcus aureus, which produces toxins that form larger, fluid-filled blisters — often on the trunk, arms and legs. The blisters are typically larger than in non-bullous impetigo and burst more slowly, leaving thinner, yellow crusts.
What does impetigo look like?
Common signs of impetigo include:
- Red, irritated patches: Especially around the mouth, nose and other exposed areas of the face.
- Honey-coloured or yellow crusts: The most recognisable sign. These crusts form when the blisters burst.
- Itching and discomfort: Especially around the affected areas, although itching is typically milder than in other skin conditions.
- Swollen lymph nodes: In some cases, the lymph nodes near the infection may become swollen and tender.
Why does impetigo happen?
Impetigo occurs when bacteria enter the skin through a break in the skin barrier. Even minor injuries can give bacteria access:
Entry points for bacteria
Skin injuries such as cuts, scrapes, insect bites and even small cracks in the skin give bacteria the opportunity to enter. Eczema and other chronic skin conditions also weaken the skin barrier and increase the risk. In children, it is particularly common for impetigo to develop after vigorous scratching of itchy skin.
Routes of transmission
Impetigo spreads through direct contact with an infected person. The bacteria can also be transferred via contaminated objects such as towels, washcloths, bedding and toys. This is particularly relevant in nurseries, schools and close home environments.
Who gets impetigo?
Impetigo can affect anyone, but certain groups are particularly vulnerable:
- Children between 2 and 6 years: This is the most commonly affected group, primarily due to frequent physical contact in play, minor injuries and frequent scratching.
- Children in institutions: Nurseries and schools are classic environments for impetigo outbreaks due to the close contact between children.
- People with eczema or dermatitis: The damaged skin barrier gives bacteria easier access to colonise and infect the skin.
- People with weakened immune systems: A weakened immune system makes it harder for the body to fight off bacterial infections.
What can you do about impetigo?
Impetigo is typically treated with antibiotics. The choice of treatment depends on the extent and location of the infection:
💊 Over-the-counter treatment (mild impetigo)
For mild impetigo, wash the affected areas with soap and water and gently remove the crusts. An antiseptic cream (e.g. with hydrogen peroxide) can help reduce bacteria.
🩺 Prescription treatment (widespread impetigo)
For more widespread impetigo, doctors typically prescribe a topical antibiotic cream (e.g. fusidic acid or mupirocin). For bullous impetigo or spread, oral antibiotics may be necessary.
🧴 Hygiene and isolation
Keep the affected area clean and covered. Avoid sharing towels, washcloths and bedding. Wash hands frequently and keep the child home from nursery until 24 hours after starting treatment.
Medical classification: Impetigo is classified as 1B72 in the WHO's International Classification of Diseases (ICD-11). It is a bacterial skin infection presenting with honey-coloured crusted lesions.
Frequently asked questions
Is impetigo dangerous?
Impetigo is rarely dangerous in healthy children and adults and is normally treated effectively with antibiotics. Untreated impetigo can, however, in rare cases lead to deeper skin infections or kidney problems (post-streptococcal glomerulonephritis).
How do I prevent impetigo?
Good hand hygiene is key. Wash hands regularly with soap, avoid sharing personal items such as towels, and keep small cuts and scrapes clean and covered. If your child has eczema or itchy dermatitis, keeping nails short and itch under control is important.
When should I contact a doctor?
Contact a doctor or dermatologist if impetigo does not improve with over-the-counter treatment within a week, if the infection spreads rapidly, or if your child develops a fever or swollen lymph nodes.
Get a diagnosis within 48 hours
Unsure about your or your child's skin condition? Upload photos via the SKIND app and receive a personal assessment and treatment plan from a certified dermatologist.
Disclaimer: This article is for informational purposes only and does not replace professional medical advice. Always consult a doctor or dermatologist for personal guidance.