What is Contact Dermatitis? Causes, Symptoms and Treatment
SkinChange.AI
Medical editorial team
Contact dermatitis is one of the most common skin conditions, occurring when the skin reacts to a substance it has touched. It can affect anyone — regardless of age or skin type — and presents as redness, itching, blisters or dryness on the affected areas.
In this article, we explain exactly what contact dermatitis is, the two main types that exist, what it looks like, and what you can do about it.
What is contact dermatitis?
Contact dermatitis is an inflammatory skin condition that arises as a direct reaction to a substance the skin has touched. Unlike atopic eczema (atopic dermatitis), contact dermatitis is not genetically determined — it is always caused by an external trigger. This means that if you can identify and remove the trigger, symptoms often disappear.
There are two main types of contact dermatitis, and it is important to distinguish between them as treatment may vary:
- Irritant contact dermatitis: The most common type. Occurs when a substance directly damages the skin's protective barrier — regardless of whether you have been exposed to it before. Anyone can develop it with sufficient exposure.
- Allergic contact dermatitis: An immune reaction in which the body's immune system reacts to a specific allergen you have previously been sensitised to. Only people with this specific sensitivity develop symptoms.
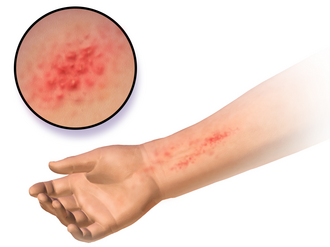
What does contact dermatitis look like?
Symptoms vary depending on the type and severity of the reaction, but common signs include:
- Redness and inflammation: Affected areas may appear red, swollen and warm to the touch.
- Itching and burning: Intense itching, burning or stinging sensations are typical.
- Blisters and bumps: In some cases, small blisters or bumps may develop on the affected skin.
- Dryness and scaling: Chronic exposure can lead to dry, cracked and scaly skin.
Contact dermatitis typically appears on the hands, wrists, arms and face — areas most often in contact with irritant substances. The reaction is often limited to the area that has been in direct contact with the trigger, but in allergic cases it can spread to other areas.
Why does contact dermatitis happen?
The cause depends on the type:
Irritant contact dermatitis
Irritant contact dermatitis occurs when a substance directly damages the outermost protective layer of the skin — the epidermis. The damage disrupts the barrier function and triggers inflammation. The stronger the irritant and the longer the exposure, the greater the risk.
Common irritants include soaps, detergents, solvents, oils, acids, alkalis and plants such as nettles. Even repeated water exposure — for example frequent hand washing — can dry out the skin and lead to irritant dermatitis.
Allergic contact dermatitis
Allergic contact dermatitis involves a delayed immune reaction (Type IV hypersensitivity) in which the immune system is activated against a specific allergen. The reaction may take 24–72 hours to manifest after exposure.
Common allergens include nickel (in jewellery and metal parts), fragrances, cosmetics, latex, certain medications, balsam and resins from plants. Even products you have used for years can suddenly trigger an allergic reaction, as sensitisation can develop over time.
Who gets contact dermatitis?
Anyone can develop contact dermatitis, but certain factors increase susceptibility:
- Frequent exposure to chemicals: Healthcare workers, hairdressers, cleaning staff and mechanics are particularly exposed.
- Underlying skin conditions: People with atopic eczema have a weakened skin barrier and are more susceptible.
- Specific allergens: Nickel allergy is among the most common contact allergies worldwide.
- Occupations with high exposure: Hairdressers, laboratory workers, metalworkers, healthcare workers and agricultural workers have elevated risk.
What can you do about contact dermatitis?
Contact dermatitis is manageable, and in most cases symptoms disappear once the trigger is identified and removed. The key to success is a combination of avoidance, skincare and medical treatment:
🔍 Identify and avoid the trigger
This is the most important step. Keep a diary of symptoms and activities, and discuss patch testing with a dermatologist to identify specific allergens.
🧴 Protect the skin
Wear protective gloves when handling chemicals. Moisturise the skin regularly with fragrance-free moisturisers to strengthen the barrier function.
💊 Medical treatment
Corticosteroid creams or ointments are the standard treatment for inflammation and itching. For severe allergic dermatitis, a dermatologist may recommend a shorter course of a stronger topical steroid or other medications.
🚿 Gentle skincare
Avoid soaps with fragrance and surfactants. Use lukewarm water instead of hot water, and avoid rubbing the skin dry. Choose cleansers and moisturisers formulated for sensitive skin.
Medical classification: Contact dermatitis is classified as ED60 in the WHO's International Classification of Diseases (ICD-11). Irritant contact dermatitis accounts for approximately 80% of all cases. Treatment is based on identification and avoidance of the trigger plus topical steroids.
Frequently asked questions
Is contact dermatitis contagious?
No, contact dermatitis is not contagious and cannot be spread from person to person. It is a local skin reaction to an irritant substance or allergen.
When should I contact a dermatologist?
Contact a dermatologist if the rash is extensive, does not improve after a week of avoidance, worsens significantly, or if you suspect a specific allergen that needs to be identified through patch testing.
How do I prevent contact dermatitis?
Prevention is about minimising contact with known irritants and allergens. Wear protective gloves, choose fragrance-free products, and keep the skin moisturised with gentle creams to strengthen the barrier function.
Get a diagnosis within 48 hours
If you have a persistent skin rash you cannot identify, you can get a personal assessment from a certified dermatologist via the SKIND app — with no waiting list.
Disclaimer: This article is for informational purposes only and does not replace professional medical advice. Always consult a dermatologist for personal guidance.